This web page was produced as an assignment for Genetics 564, a capstone course at UW- Madison.
What is tyrosinemia?
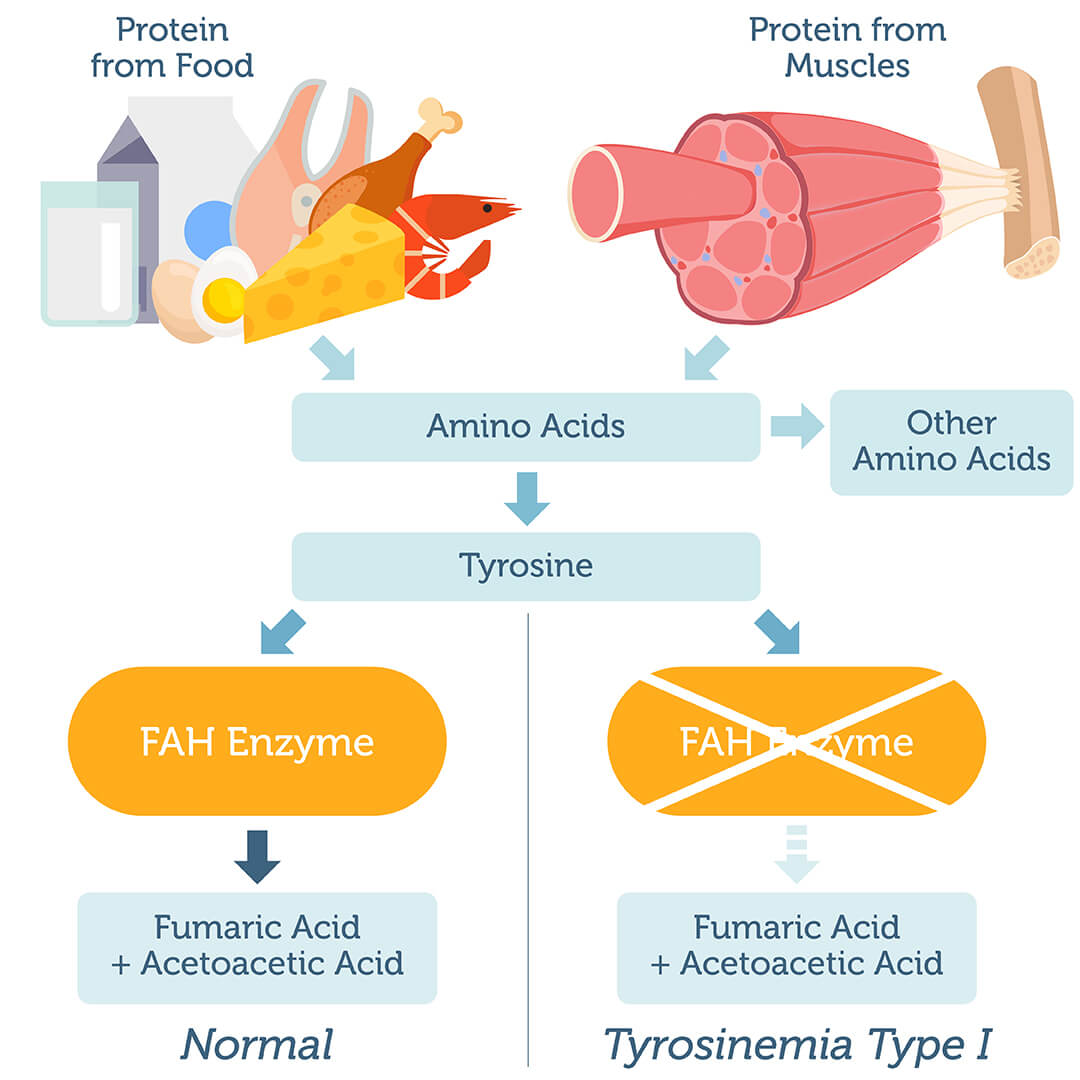
Tyrosinemia is a rare genetic disorder that is characterized by the inability to breakdown the amino acid tyrosine in the body, leading to a buildup of tyrosine and it's byproducts that when left untreated, cause severe consequential health issues. [1] Tyrosine is a common component of most proteins, so when proteins are broken down in the body tyrosine is unable to be metabolized and the buildup begins to cause damage in the liver, where tyrosine is normally metabolized, as well as the kidneys. There are three different types of tyrosinemia (I, II, III) and each is classified by a mutation in different genes that cause different enzymes that break down tyrosine in the body to be absent. There are many mutations in the FAH gene that can cause tyrosinemia type 1 and it is unknown how each interact with each other.
types of tyrosinemia
|
TYPE 1 Tyrosinemia Type 1 is characterized by a mutation in the FAH gene, located on chromsome 15, which encodes for the enzyme fumarylacetoacetate hydrolase. [3] Without this enzyme, tyrosine is unable to be broken down and builds up in the liver. |
|
TYPE 2
Tyrosinemia Type 2 is characterized by a mutation in the TAT gene, that encodes the enzyme tyrosine aminotransferase. |
TYPE 3
Tyrosinemia Type 3 is characterized by a mutation in the HPD gene, which encodes the enzyme 4-hydroxyphenyl-pyruvate dioxygenase |
symptoms / signs of tyrosinemia type 1
|
Tyrosinemia Type 1 presents in two ways, acute and chronic. Acute tyrosinemia is more severe and presents itself at birth or a few months after while chronic tryosinemia has a gradual onset of symptoms, usually less severe then the acute form. [4] Early symptoms include :
|
|
inheritance
Tyrosinemia Type I is an autosomal recessive genetic disorder, meaning that in order to inherit this disease, one must get a mutated copy of the gene from each parent. There is no increased risk in terms of gender, however there are differences in numbers distributed geographically. Worldwide, the number of affected individuals is ~ 1 in 100,000 births, while in Quebec, Canada it is ~ 1 in 16,000 births and in certain regions of Quebec is as high as ~ 1 in 1,850 births. [5]
testing and treatment options
There are a few ways to test for tyrosinemia type 1, including blood tests, tandem mass spectroscopy, and genetic testing. Most states in the U.S. screen for tryosinemia upon birth through tandem mass spectroscopy, which takes newborn blood spots and looks for succinylacetone, which is found when the enyzme fumarylacetoacetate hydrolase is not functioning properly. [4] There is also genetic testing that can be performed to look at the FAH gene as well as genetic counseling which can help families that knowingly carry this mutation assess the possibilities/risks of birth. [5]
|
If diagnosed early enough, there is a treatment option with the drug Nitisinone, which prevents the buildup of these tyrosine byproducts and has been proven effective in most, reducing the need for liver transplants that were previously crucial for survival of this disorder. Along with this drug, low tyrosine diets (low protein) and other dietary restrictions are also recommended in order to maintain optimal liver function. Approximately 90% of children respond to Nitisinone and diet changes, however there are some cases, such as if liver cancer is suspected or if acute tyrosinemia has progressed, that liver transplant is necessary. [2]
|
|
to learn more about tyrosinemia type 1, visit these links ...
references
[1]Bethesda (MD): National Library of Medicine (US); MedlinePlus [Internet]. [updated 2020 Jun 24]. Noonan syndrome; [updated 2020 Jun 18; reviewed 2018 Jun 01; cited 2020 Jul 1]; [about 5 p.]. Available from:
https://medlineplus.gov/genetics/condition/tyrosinemia/#:~:text=Tyrosinemia%20is%20a%20genetic%20disorder,lead%20to%20serious%20health%20problems.
[2]Children’s Pittsburgh (updated 2024) : Tyrosinemia symptoms & treatment. Children’s Hospital of Pittsburgh. (n.d.). https://www.chp.edu/our-services/transplant/liver/education/liver-disease-states/tyrosinemia#:~:text=The%20treatment%20for%20tyrosinemia%20is,and%20beans%20should%20be%20avoided
[3[King, L. S. (2017, May 25). Tyrosinemia type I. GeneReviews® - NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK1515/#:~:text=Tyrosinemia%20type%20I%20is%20caused,see%20Figure%201%20and%20Pathophysiology).
[4]Kshitiz Singh, PhD, Research Fellow, The Children’s Hospital of Philadelphia, and Robert M. Tanguay, DSc, Professor and Associate Head, Department of Molecular Biology, Medical Biochemistry & Pathology, Lab Cell & Developmental Genetics, Universite Laval, Quebec, Canada ; National Organization for Rare Disorders. (2023, November 20). Tyrosinemia type 1 - Symptoms, causes, treatment | NORD. https://rarediseases.org/rare-diseases/tyrosinemia-type-1/
[5]Paradis K. (1996). Tyrosinemia: the Quebec experience. Clinical and investigative medicine. Medecine clinique et experimentale, 19(5), 311–316.
https://medlineplus.gov/genetics/condition/tyrosinemia/#:~:text=Tyrosinemia%20is%20a%20genetic%20disorder,lead%20to%20serious%20health%20problems.
[2]Children’s Pittsburgh (updated 2024) : Tyrosinemia symptoms & treatment. Children’s Hospital of Pittsburgh. (n.d.). https://www.chp.edu/our-services/transplant/liver/education/liver-disease-states/tyrosinemia#:~:text=The%20treatment%20for%20tyrosinemia%20is,and%20beans%20should%20be%20avoided
[3[King, L. S. (2017, May 25). Tyrosinemia type I. GeneReviews® - NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK1515/#:~:text=Tyrosinemia%20type%20I%20is%20caused,see%20Figure%201%20and%20Pathophysiology).
[4]Kshitiz Singh, PhD, Research Fellow, The Children’s Hospital of Philadelphia, and Robert M. Tanguay, DSc, Professor and Associate Head, Department of Molecular Biology, Medical Biochemistry & Pathology, Lab Cell & Developmental Genetics, Universite Laval, Quebec, Canada ; National Organization for Rare Disorders. (2023, November 20). Tyrosinemia type 1 - Symptoms, causes, treatment | NORD. https://rarediseases.org/rare-diseases/tyrosinemia-type-1/
[5]Paradis K. (1996). Tyrosinemia: the Quebec experience. Clinical and investigative medicine. Medecine clinique et experimentale, 19(5), 311–316.
This web page was produced as an assignment for Genetics 564, a capstone course at UW-Madison.